Alveolar Ridge Preservation: How to Perform Socket Preservation Techniques

Table of Contents
Talking about alveolar ridge preservation (or socket preservation) always reminded me of a story about an American comedian performing a gig in New York City.
He walked onto the stage in a good mood and started to show his best material and jokes, producing his best performance.
But nobody was laughing.
He kept on trying, but there was no result. Nothing.
He walked off the stage and thought about quitting being a comedian.
Then he discovered that the audience was an Italian tour group, and no one understood a word of English.
Was he a bad comedian after all?
Should he try the same jokes in another gig and this time with English-speaking people?
For sure, he should.
Why is this similar to performing ridge preservation?
This reminds me that sometimes when a given technique is performed using specific materials on a given patient, the outcome does not turn out as expected because the method, or the background, was not indicated.
And this applies especially to ridge preservation.
Discussing the preservation of the alveolar ridge is like discussing marketing. Everyone has his own opinion about it and often has no scientific background to support what they or say.
Therefore, if we try to explain in two sentences what ridge preservation is, we will likely find ourselves stuck in the middle of it or guessing and wondering if what we just said is supported by scientific publications.
I should perform an alveolar ridge if
_________________________________________.
And use this special technique if
_________________________________________.
This article focuses on filling these two sentences and explaining the basic techniques to perform ridge preservation.
What does it look like after an extraction, and why is it important to perform alveolar ridge preservation?
It was already described here on Periospot what happens after extraction and the timing to place an implant after socket preservation. With this animation is easier to understand why there is bone loss after an extraction.
Based on Cardaropoli's article about alveolar bone dynamics after an extraction, this animation explains the events that occur (Cardaropoli 2003) and what process is expected in the alveolar bone.
Bone resorption after extraction: Is it due to raising the flap or the loss of irrigation to the bundle bone?
Various surgical strategies have been developed to preserve the alveolar ridge, reduce bone loss, improve socket healing, and incorporate diverse graft materials, resorbable membranes (or not resorbable), and flap configurations.
Despite these differences, no single approach has been definitively shown to be more successful than others, as indicated by research from Vignoletti et al. (2011).
Existing literature suggests that surgical trauma during the procedure can impact treatment outcomes. In this regard, additional research and publications have explored the significance of trauma during extractions.
Efforts to minimize trauma during surgery have been emphasized in some studies to achieve the best possible results (Fickl et al., 2008).
The significance of mucoperiosteal flap elevation during the procedure in the post-extraction site's healing process has been debated. Disrupting the osteogenic cell layer in the mature periosteum might negatively affect regenerative abilities.
However, the findings across various studies have been inconclusive. Some researchers argue that bone remodeling is effectively decreased after flapless surgeries (Fickl et al. 2008), whereas others, such as Araujo and Lindhe, have found no significant differences (2009, Barone et al. 2014).
In collaboration with Lindhe, Araujo's research has focused on the notion that volume loss following extraction is primarily due to tooth loss and not associated with flap elevation.
In their 2006 publication on immediate implants, they attempted to establish a link between flap management and post-extraction volume loss.
Additionally, their 2005 publication explored the dynamics of bone remodeling and soft tissue changes after tooth extraction. Despite their contributions, a consensus on the relationship between flap elevation and post-extraction volume loss remains elusive.
Immediate implants flapless: Blanco's publication.
In 2008, Blanco challenged the theory that associated flap elevation with post-extraction volume loss, which could have negative consequences for immediate implants.
Blanco's research aimed to debunk this idea by examining the relationship between flap elevation and the success of immediate implants following tooth extraction.
Through this investigation, Blanco provided new insights that questioned the assumptions previously held about flap management and its impact on implant success.
This contribution to the field helped stimulate further discussion and research on the topic, ultimately enhancing the understanding of factors that influence the outcome of immediate implant procedures.
Blanco's article concludes: Use narrow implants and flapless surgery in immediate implants!
Let's get back to the Ridge Preservation.
Regarding the decision to perform ridge preservation and to fill out the first sentence (I should perform alveolar ridge preservation if _____________), we should take a look at the decision tree proposed by Jung (Jung 2018):
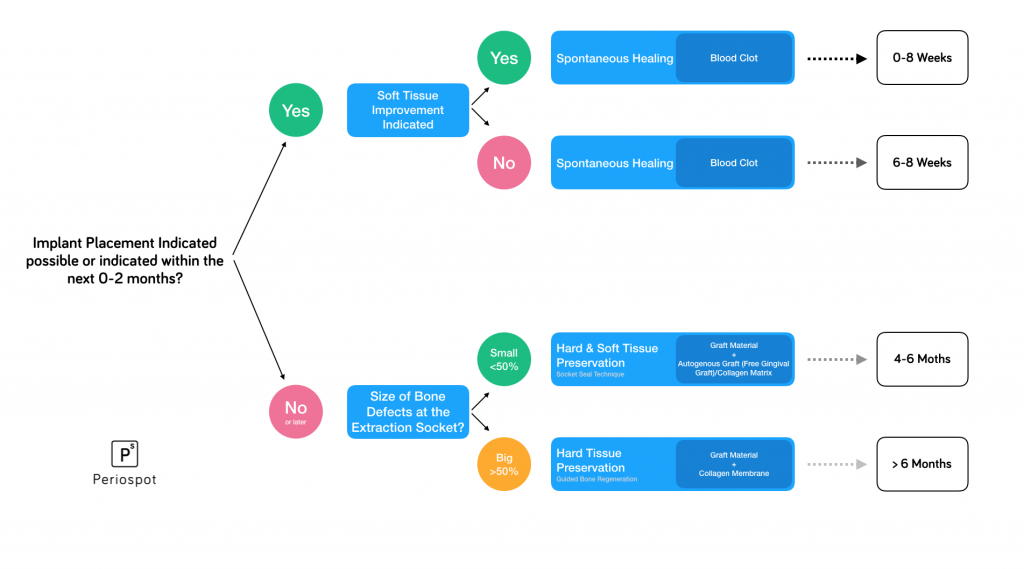
After deciding whether to perform ridge preservation, immediate implant or an immediate implant using a Socket Shield technique, early implant placement, or delayed implant placement, we should know that to perform alveolar ridge preservation to maintain the alveolar bone, there are three options:
- Using soft tissue grafts.
- Using hard tissue grafts.
- Combination of soft and hard tissue grafts.
We are going through some of these socket preservation techniques. I will also provide a different approach that was a game-changer for me and is my secret weapon.
First, it's mandatory to mention that an immediate implant is also an option. However, some publications consider it a technique to avoid if we seek an aesthetic result (Tonetti 2017).
Although the abovementioned article is a randomized controlled trial, we should read it cautiously. I explain more about this publication in this article if you want to learn more about why the author states that immediate implants are not recommended when aesthetics are at stake.
Also, to get some tips about immediate implants, don't miss this article, where I cover some guidelines on this procedure.
But let's go back to ridge preservation.
#1. Soft tissue preservation
This is indicated if we consider placing the implant in the next two months after extraction.
The main reason for performing this approach is a lack of soft tissue due to the recession.
In these cases, biomaterials are not used as they would delay bone formation and bone healing.
#2. Soft and hard tissue preservation in the ridge preservation techniques
This technique is indicated when the buccal bone defect is less than 50%, and the implant is planned to be placed after 4–6 months.
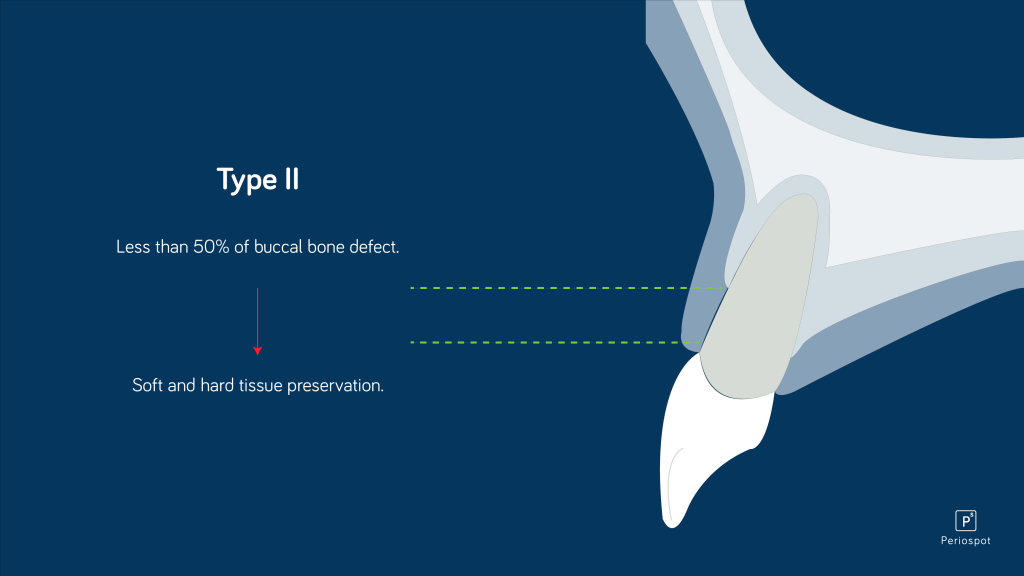
Studies have shown that performing socket preservation with a bone substitute and a soft tissue graft is reliable for preventing vertical and horizontal changes after extraction (Jung 2004).
Two techniques that can be used in these situations are the following:
1) Alveolar ridge preservation using the Ice Cone Technique
Elian proposed this technique in cases where the gingival margin is preserved but has a buccal bone defect (Elian 2007).
It is always important to check the integrity of the buccal bone, as there is sometimes no soft tissue recession. If a buccal bone defect is present, and if we perform an immediate implant in this condition, it may lead to dramatic aesthetic failure.
"This video explains the socket preservation technique using a resorbable collagen membrane acting as a"fake” bone wall to allow the xenograft placement.
Furthermore, as demonstrated in the case below, it is possible to seal it with an autogenous soft tissue graft or a collagen matrix(Jung 2013). Sealing the socket preservation will prevent the leakage and contamination of the biomaterial.
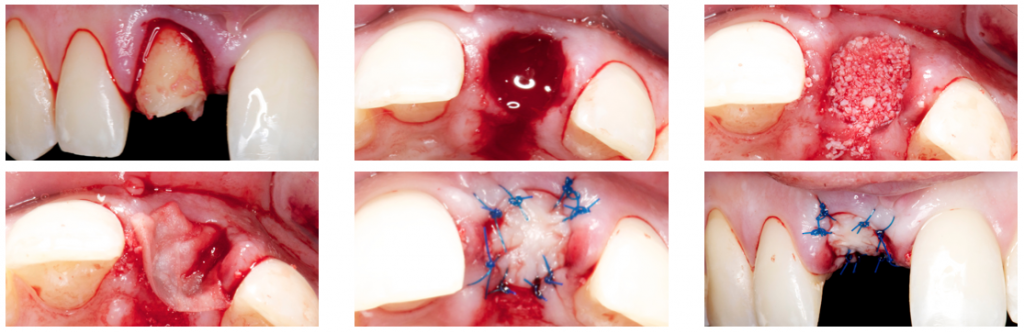
2) Stimmelmayer Technique (Stimmelmayer 2010) for socket preservation technique
This technique consists of a combination of an epithelized-subepithelial connective tissue graft.
Although it involves a socket-seal technique combined with an immediate implant, I will describe it as a dependable approach for ridge preservation.
In my opinion, this technique is superior to any other technique as it has two main advantages:
- Thickening the buccal soft tissue in advance.
- It enhances the contact between the donor site and the graft. This makes it almost impossible to have necrosis of the graft.
The result has a graft that will contract the unavoidable shrinkage of the alveolar ridge after an extraction.
The animations below show placing the combined epithelized-subepithelial connective tissue graft in a fresh extraction socket. It mainly consists of preparing two receptor chambers, one buccally and the other palatally, with partial thickness.
This animation shows the placement of a combined subepithelial and epithelial graft in the socket.
After 4–6 months, the condition of the alveolar ridge will allow proper placement of the implant. Also, we observed a nice amount of soft tissue after the socket healing.
This prevents the necessity of performing a second connective tissue graft after the socket preservation.
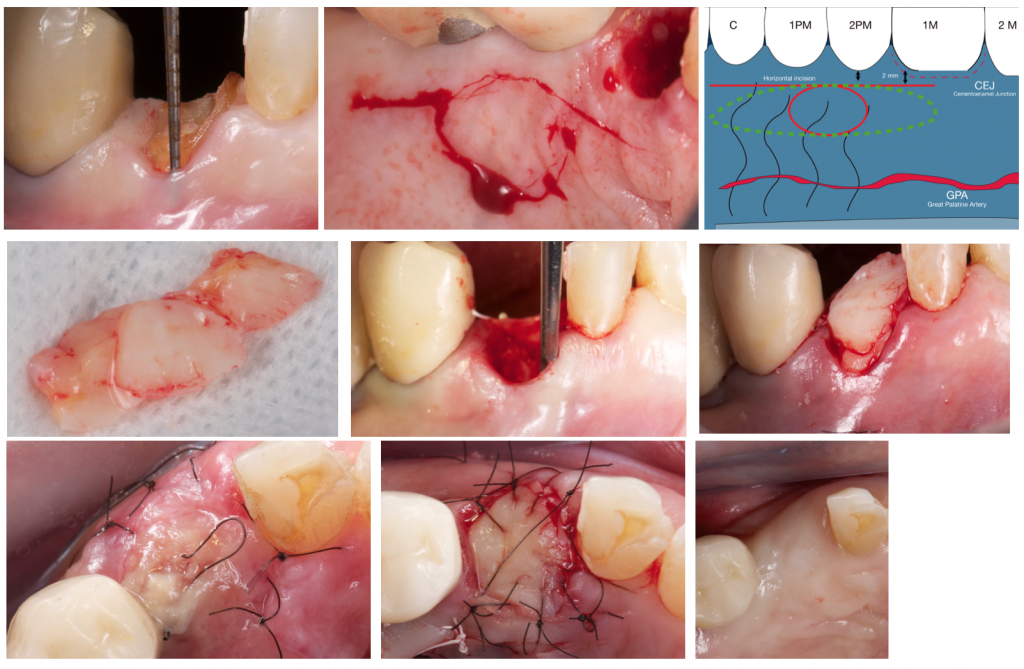
The main drawback of this technique is that harvesting an epithelized-subepithelial connective tissue graft from the palate is not technically easy.
Also, the wound at the donor site can be very uncomfortable for the patient due to the extent of the graft.
Is important to mention that in this case we did not use any collagen membrane or any other barrier membrane.
Some extra animation about the Stimmelmayer technique on this page.
#3. Hard Tissue Preservation
I once listened to a beautiful lecture about immediate implants from Albert Barroso. (I must say it was the best lecture about this topic I've ever heard.) During the lecture, Albert said:
"The other day, one of my students tried to perform socket preservation in an Elian Type III Socket. This is only effective if one wants the biomaterials company to achieve their sales target"." The other day, one of my students tried to perform socket preservation in an Elian Type III Socket. This is only effective if one wants the biomaterials company to achieve their sales target".
And he was right. Trying to preserve a ridge in a Type III socket is like convincing flat-earthers that planet earth is round.
Therefore, performing flapless socket preservation is useless when a buccal bone defect is more than 50%.
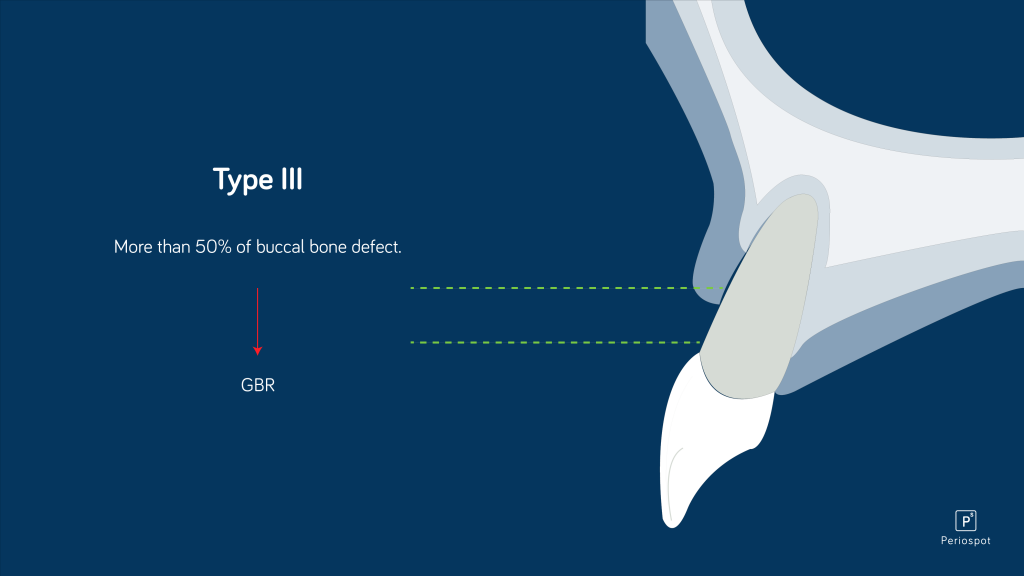
In such cases, the most effective approach is to perform guided bone regeneration using a xenograft and a resorbable membrane—finally, a coronal advancement flap to cover the bone regeneration.
In this situation, placing the graft and not covering it with a coronal advancement flap has weak evidence (Vignoletti 2012).
Advantages and benefits of extraction socket preservation (Kim 2020)
- Reduces the resorption of the alveolar bone after tooth extraction, preserving the bone volume and architecture of the ridge.
- It provides better bone quality for implant placement, improving the implant survival rate and long-term stability.
- Reduces the need for additional bone augmentation procedures, which can be costly and time-consuming.
- Reduces the need for soft tissue augmentation procedures, improving aesthetic outcomes.
- It can be performed immediately after extraction, reducing the overall treatment time.
- It can be performed with a variety of materials, including autogenous bone, allografts, xenografts, and synthetic bone substitutes.
- It has a high success rate and low complication rate when performed by experienced clinicians.
Conclusion about alveolar ridge preservation
Similarly, having a comedian friend with great jokes or a doctor who uses the best biomaterials and has outstanding surgical skills does not guarantee the success of alveolar ridge preservation.
As this article summarizes, it is crucial to use a decision tree to choose the appropriate approach in cases where immediate implant placement is not recommended.
It is essential to make some takeaway remarks regarding alveolar ridge preservation:
- Performing ridge preservation will provide more optimal conditions for ideal implant placement. It is always better to preserve than leave the socket to heal spontaneously.
- Patients can undergo implant surgery four months after alveolar ridge preservation. We have already reviewed the literature and this infographic. You can find that after four months, there are already conditions for implant installment (de Rissi 2014).
- Consider the two months of osseointegration as a part of the graft maturation process in the alveolar ridge preservation.
- Covering the biomaterial with an autogenous soft tissue or a soft tissue substitute will provide a superior outcome (Jung 2013).
- Alveolar ridge preservation can augment the volume of soft and hard tissue if necessary, using guided bone regeneration, connective tissue graft (for extensive soft tissue defects), or a roll technique (for minor soft tissue defects).
- Alveolar ridge preservation will not avoid the resorption of the bundle bone. The thinner buccal alveolar bone wall will always be resorbed until it is at least 1,8 mm thick (Spray 2000). Therefore, the only way to preserve the buccal bone wall is with a Socket Shield Technique.
- There is the most chance of efficient alveolar ridge preservation in molars due to the width of the buccal bone wall.
- Suturing techniques also play an important role in alveolar ridge preservation. Check this article to get more insights about suturing techniques in implant dentistry.
- Primary closure of the socket is difficult unless you raise a flap.
- Always double-check other articles and keep your critical thinking about scientific publications.
Closing remarks about socket preservation
Although alveolar ridge preservation is a vast topic, I tried to summarize in this article what the scientific literature says about this approach and also my clinical experience with alveolar ridge preservation in the past 14 years.
Today, if I had to pick a favorite technique, I would undoubtedly choose the Stimmelmayer approach.
I hope you find this helpful article and, as always. I would love to hear your feedback and questions about this topic.
Also, check the other fantastic article we published on Periospot about this same topic but more focused on the soft tissue.
Recommended Book- Plastic- Esthetic Periodontal and Implant Surgery

Bibliographic references:
- Cardaropoli, D., Tamagnone, L., Roffredo, A., & Gaveglio, L. (2003). Dynamics of bone tissue formation in tooth extraction sites: An experimental study in dogs. Journal of Clinical Periodontology, 30(9), 809-818.
- Jung, R. E. (2018). Decision-making criteria for alveolar ridge preservation in daily practice. European Journal of Oral Implantology, 11(Suppl 1), S91-S101.
- Jung, R. E., Sailer, I., & Hämmerle, C. H. (2013). Attitudes of dental professionals towards implant-based complete-arch reconstructions for the edentulous jaw. International Journal of Prosthodontics, 26(2), 117-119.
- Jung, R. E., Zembic, A., Pjetursson, B. E., Zwahlen, M., & Thoma, D. S. (2017). Systematic review of the survival rate and incidence of biologic, technical, and aesthetic complications of single implant abutments supporting fixed prostheses. International Journal of Oral and Maxillofacial Implants, 32(2), 299-311.
- Elian, N., Cho, S. C., Froum, S., Smith, R. B., Tarnow, D. P., & Rosenberg, E. (2007). Real-time, in vivo evaluation of immediate implant placement and provisionalization in anterior single-tooth replacement. Journal of Periodontology, 78(9), 1596-1601.
- Stimmelmayr, M., Allen, E. P., Reichert, T. E., Klotz, M. W., & Bornstein, M. M. (2010). An epithelized subepithelial connective tissue graft technique for soft tissue augmentation at implant sites: A pilot study. Journal of Periodontology, 81(2), 239-246.
- Jung, R. E., & Thoma, D. S. (2012). The socket-shield technique. Implant Dentistry, 21(1), 2-8.
- Vignoletti, F., Discepoli, N., Müller, R., De Sanctis, M., & Sanz, M. (2012). Immediate versus delayed single-tooth implant placement after anterior maxillary tooth extraction: Literature review. European Journal of Oral Implantology, 5(Suppl), S71-S89.
- de Risi, V., Clementini, M., Vittorini Orgeas, G., Mannocci, A., & De Sanctis, M. (2014). Surgical techniques for alveolar ridge preservation: A systematic review. Clinical Oral Implants Research, 25(3), 240-254.
- Spray, J. R., Black, C. G., & Morris, H. F. (2000). The influence of bone thickness on facial marginal bone response: Stage 1 placement through stage 2 uncovering. Annals of Periodontology, 5(1), 119-128.
Check Your Knowledge
Comments
0 totalLoading comments...
Previous
How Deep Is Your Implant? Supracrestal, Crestal, and Subcrestal Implant Position Revisited.
Next
How Dentists value immediate returns and their relationship to the human brain and digital dentistry
Related Articles

Dental KOL Marketing: How Implant and Periodontal Brands Build Their Key Opinion Leader Bench
11 min read
Dental Video Marketing: How Brands Use Clinical Video to Drive KOL Adoption
12 min read
