Immediate Implants in the Aesthetic zone: Some tips and tricks that will help you

Table of Contents
When I'm in the middle of a discussion about the topic of immediate implants, I always remember Schulte.
Schulte was the first to describe the placement of the immediate implants as a different therapeutic approach (Schulte 1976).
But I can imagine how much he was criticized at the moment when the only accepted approach was the Branemark protocol.
If you support the 3-6 months loading protocol, maybe you should consider stopping reading this article right now.
I´m serious! I mean it.
Also, I can imagine the scientific community at the time mocking the Schulte approach, like this guy from Microsoft:
"500 Dollars for a phone, and it even doesn't have a keyboard"?????? Yep, he nailed it!

Also, I wanted to do a small experiment with dentists, and I did a poll on Twitter:
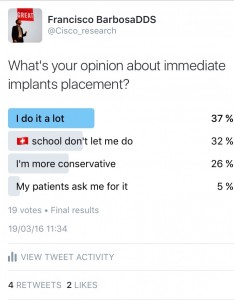
And guess what? It seems we do like the immediate implants approach...
But let´s start with the serious stuff now.
Does it work? Is it a reliable option? When can we perform it? Well, questions about this topic are finite, but there may be many of them to solve in a blog post.
But there are too many to answer in just a blog post
So let´s try to brainstorm around it.
Diagnosis: Case selection is the key to success.
To have an accurate assessment of a case, you should try the ERA Tool- Esthetic Risk Assessment Tool (Cordaro 2009).
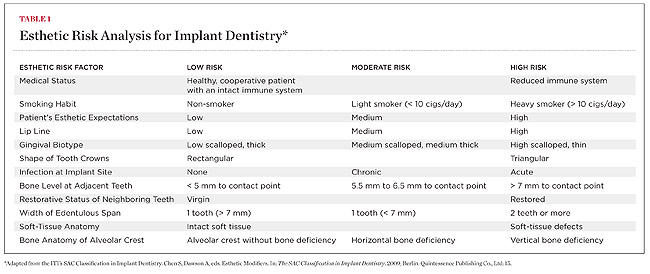
I created my own Excel, where I can have an idea of the case I have in front of me is complex, straightforward, or advanced. It looks like this:

Then I count how many red, green, or yellow boxes I have.
It is essential to see how many red boxes outweigh the green, which makes this case unsuitable for an immediate case for greater predictability; it's far more essential to have more green boxes.
Also, I focus on three critical points.
1) The lip line. This will determine if any mistake you may commit will be visible
2) The soft tissue biotype: I´ll write about this later, but to have an idea, the recession is more likely to happen in a thin biotype (Kan 2011)
3) The patient's expectation. Make sure that the outcome that the patient seeks is possible from a biological and functional point of view.
Also, be aware of the patient´s girlfriend, mother,, or other relative expectations. I once had an unscheduled quarrel with a patient relative, and it was not a pleasant experience.
Socket anatomy and morphology
We have to check always the integrity of our sockets.
"The presence of interproximal bone is mandatory if you want to get some papilla around the restoration (Kan 2003)."
The presence of the buccal bone will determine if you should perform a more conservative approach. The Elian classification is useful in this case (Elian 2007):
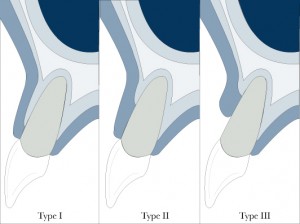
Type I socket is favorable for an immediate implant placement, while type II and Type III will need an augmentation procedure.
If we use a CT scan (which is strongly recommended), we can check the sagittal root position concerning the anterior maxillary osseous housing.
Watch this video to learn the classification:
In a nutshell: The type I socket is the most favorable and the most common, with around 81% in a sample size of 600 patients (Kan 2011).
Surgical tips
Choosing the right implant
This is a controversial point, so I´m going to try to be polite.
Primary stability has been suggested to be an essential prognostic for osseointegration (Brunski 1988).
There are also publications where implants without primary stability could be osseointegrated when they were left undisturbed during the healing process (Ivanoff 1996, Rodrigo 2010).
"It is, in fact, important to achieve optimal primary stability if we are going to perform an immediate restoration."
But did you know that even a 10 N·Cm torque would be enough as long as the provisional is bonded to the adjacent teeth? (Norton 2011)
I cannot recommend you load an implant that was placed with a torque of 10 N·Cm. Please, read some guidelines regarding immediate loading in this article.
You´ll feel more confident if a higher torque is achieved during the implant placement. Higher torque means a higher survival rate and also fewer complications (Ottoni 2005).
So, what's the best implant geometry for an immediate implant?
A conical implant seems to achieve more optimal primary stability in a fresh extraction socket (Kan 2014). However, we must know that the spontaneous filling of the gap is significantly better in cylindrical implants than in conical (Tomasi 2010).
Implant diameter
If we read some articles about immediate implants, we may notice that some authors used to choose implants with a diameter of up to 5 mm (Kan 2001).
It has been shown that this can negatively affect the stability of the peri-implant soft and hard tissues (kan 2011).
That´s why the implant diameter must be chosen regarding the buccal-palatal width rather than the mesiodistal distance. The implant diameter in the anterior maxilla should be <4.5 mm.
Implant position
3D implant position is crucial to achieving an aesthetic outcome.
I´m not going to explain here the basic rules about the ideal placement of an implant in immediate cases; this has been described and illustrated in this iBook (Spanish version here).
But I created this video where some new concepts are explained:
We have to avoid our implant to be drifted buccally. That is important that during the drilling, we should start drilling in the palatal wall, avoiding the root tip.
This will provide an ideal position to restore the implant, an ideal gap between the implant and the buccal wall.
Avoiding the buccal wall also will save us a lot of biological complications.
Remember: Never engage the implant to the buccal wall. Never!
Using an SCTG simultaneously for immediate implant placement
It is well described in the literature that using a subepithelial connective tissue graft simultaneous to immediate implant placement improves the stability of the peri-implant soft tissue (Cornelini 2008, Kan 2009, Chung 2011, Tsuda 2011).
Compared to immediate implants without connective tissue graft, SCTG was beneficial in maintaining the facial gingival level (Yoshino 2014).
Prosthetic tips
The use of a provisional
I have written about the importance of using temporaries in this free ebook about aesthetic implant dentistry.
They are essential if we seek an aesthetic outcome. Regarding immediate implants, some authors have suggested that the provisional is essential to maintain the dentogingival architecture (Yoshino 2014).
At this point, I would like to add that using a CAD/CAM PMMA may be the best option, as they have been proven to have optimal mechanical and biological behavior (Edelhoff 2012).
I advocate for the PMMA CAD/CAM restorations, which I´ve already described as an essential part of my workflow when I perform a Digital Socket Shield Technique (iBook here).
Prosthetic Emergence Profile
Concave emergence profiles seem to have a positive impact.
Several authors have already tested this feature (Rompen 2007, Redemagni 2009). Also, we should consider using a definitive abutment placed on the same day of the surgery to avoid further disconnections (Abrahamsson 1997).
Let´s see how this concave profile can be applied, illustrated with this short video (Su 2011):
Conclusions
Although this is a controversial topic, I feel these points can be helpful from a clinical point of view:
We could conclude that using SCTG is mandatory for thin biotypes.
Also, provisional use is a "must-have" in every restoration with a demanding aesthetic outcome.
Of course, we cannot forget that everything explained before does not make sense if the implant is not placed in an ideal 3D position.
The trimodal approach (immediate implant, flapless, immediate restoration) is a reliable and predictable procedure (Cabello 2012). In some cases, other techniques and features can be added to this approach:
- Subepithelial connective tissue graft, in a case of a thin biotype.
- Incorporate PMMA CAD/CAM provisionals.
- Socket shield technique (we have to see if this approach is predictable in the long term).
It can be an individualized approach by every clinician who incorporates scientifically based knowledge.
Do you agree with the immediate implant approach?
Do you have any tips you would like to share?
I also would like you to look at these fantastic surgery videos from Juan Alberto Fernandez (he also has this two more videos that you´ll like to see in video 2 & video 3).
In case you are interested in immediate implants in the molar zone, this article or this one with also prosthetic emphasis will provide you with some valuable guidelines.
Recommended iBook about Immediate Implants

Bibliography:
Abrahamsson I, Berglundh T, Lindhe J. The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol 1997;24:568-572.
Brunski JB. Biomaterials and biomechanics in dental implant design. Int J Oral Maxillofac Implants 1988;3:85–97.
Cabello G, Rioboo M, Fabrega JG. Immediate placement and restoration of implants in the aesthetic zone with a trimodal approach: Soft tissue alterations and its relation to gingival biotype. Clin Oral Implants Res 2012
Chung S, Rungcharassaeng K, Kan JY, Roe P, Lozada JL. Immediate single tooth replacement with subepithelial connective tissue graft using platform switching implants: A case series. J Oral Implantol 2011;37:559–569.
Cornelini R, Barone A, Covani U. Connective tissue grafts in postextraction implants with immediate restoration: A prospective controlled clinical study. Pract Proced Aesthet Dent 2008;20:337–343.
Cordaro L. Implants for restoration of single tooth spaces in areas of high esthetic risk. In: Dawson A, Chen S, Buser D et al., eds. The SAC Classification in Implant Dentistry. Quintessence Publishing; 2009:50-56
Edelhoff DD, Beuer FF, Schweiger JJ, Brix OO, Stimmelmayr MM, Guth J-FJ. CAD/CAM-generated high-density polymer restorations for the pretreatment of complex cases: a case report. Quintessence Int (Berl). 2012 May 31;43(6):457–67.
Elian N, Cho SC, Froum S, Smith RB, Tar- now DP. A simplied socket classication and repair technique. Pract Proced Aesthet Dent 2007;19:99–104.
Ivanoff CJ, Sennerby L, Lekholm U. Influence of initial implant mobility on the integration of titanium implants. An experimental study in rabbits. Clin Oral Implants Res 1996;7:120–127.
Kan JYK, Rungcharassaeng K: Site development for anterior implant esthetics: The dentulous site. Compend Cont Educ Dent 22:221, 2001
Kan JY, Rungcharassaeng K, Umezu K, Kois J. Dimensions of peri-implant mucosa: An evaluation of maxillary anterior single implants in humans. J Periodontol 2003;74:557–562.
Kan, J. Y., Rungcharassaeng, K., Lozada, J. L. & Zimmerman, G. (2011) Facial gingival tissue stability following immediate placement and provisionalization of maxillary anterior single implants: a 2- to 8-year follow-up. International Journal of Oral and Maxillofacial Implants 26, 179–187.
Kan JY, Rungcharassaeng K, Morimoto T, Lozada J. Facial gingival tissue stability following connective tissue graft with single im- mediate tooth replacement in the esthetic zone: Consecutive case report. J Oral Maxillofac Surg 2009;67:40–48.
Kan JYK, Roe P, Rungcharassaeng K, Patel RD, Waki T, Lozada JL, et al. Classification of sagittal root position in relation to the anterior maxillary osseous housing for immediate implant placement: a cone beam computed tomography study. Int J Oral Maxillofac Implants. 2011 Jul;26(4):873–6.
Kan JY, Roe P, Rungcharassaeng K. Effects of Implant Morphology on Rotational Stability During Immediate Implant Placement in the Esthetic Zone. Int J Oral Maxillofac Implants. 2014 Dec 31;30(3):667–70.
Norton, M.R. (2011) The influence of insertion torque on the survival of immediately placed and restored single-tooth implants. The International Journal of Oral & Maxillofacial Implants 26: 1333–1343.
Ottoni JM, Oliveira ZF, Mansini R, Cabral AM. Correlation between placement torque and survival of single-tooth implants. Int J Oral Maxillofac Implants 2005;20:769–776.
Redemagni M, Cremonesi S, Garlini G, Maiorana C. Soft tissue stability with immediate implants and concave abutments. Eur J Esthet Dent 2009;4:328–337.
Rompen E, Raepsaet N, Domken O, Touati B, Van Dooren E. Soft tissue stability at the facial aspect of gingivally converging abutments in the esthetic zone: A pilot clinical study. J Prosthet Dent. 2007 Jun;97(6):S119–25.
Rodrigo, D., Aracil, L., Martin, C. & Sanz, M. (2010) Diagnosis of implant stability and its impact on implant survival: A prospective case series study. Clinical Oral Implants Research 21: 255–261.
Schulte W, Heimke G. The Tubinger immediate implant. Quintessenz 1976: 27: 17–23.
Tomasi C, Sanz M, Cecchinato D, Pjetursson B, Ferrus J, Lang NP, Lindhe J. Bone dimensional variations at implants placed in fresh extraction sockets: a multilevel multivariate analysis. Clin Oral Impl Res 2010: 21: 30–36.
Tsuda H, Rungcharassaeng K, Kan JY, Roe P, Lozada JL, Zimmer- man G. Peri-implant tissue response following connective tissue and bone grafting in conjunction with immediate single-tooth replacement in the esthetic zone: A case series. Int J Oral Maxillofac Implants 2011;26:427–436.
Yoshino S, Kan JYK, Rungcharassaeng K, Roe P, Lozada JL. Effects of Connective Tissue Grafting on the Facial Gingival Level Following Single Immediate Implant Placement and Provisionalization in the Esthetic Zone: A 1-Year Randomized Controlled Prospective Study. Int J Oral Maxillofac Implants. 2014;29(2):432–40.
Check Your Knowledge
Comments
0 totalLoading comments...
Previous
Soft Tissue Recession Around Implants – A common Complication
Next
How to perform a predictable immediate loading
Related Articles

Dental KOL Marketing: How Implant and Periodontal Brands Build Their Key Opinion Leader Bench
11 min read
Dental Video Marketing: How Brands Use Clinical Video to Drive KOL Adoption
12 min read
