The Story Behind Platform Switching

Table of Contents
Like most good things in life are accidental, Platform Switching, too, was discovered accidentally.
During the late ’80s, Nobel Biocare introduced wide-diameter Branemark implants (5mm), but their corresponding platform abutment was not easily available. Hence, Restorative dentists were compelled to use the available “standard” (3.75/4.0mm) diameter abutments.
Similarly, Implant Innovations Inc. 1991 introduced wide-diameter implants (5/6 mm) along with matching wide-diameter platforms.
After the introduction, matching diameter prosthetic components weren’t easily available. So many of those early implants were restored with standard diameter (4.1mm) of prosthetic components.
After a 5‑year period, the typical pattern of crestal bone resorption was not observed in Platform Switched implants.
Thus, the discovery of the concept was a coincidence.
The platform-switching concept was formally introduced in the literature by Lazzara, Porter, and Gardner (2006).
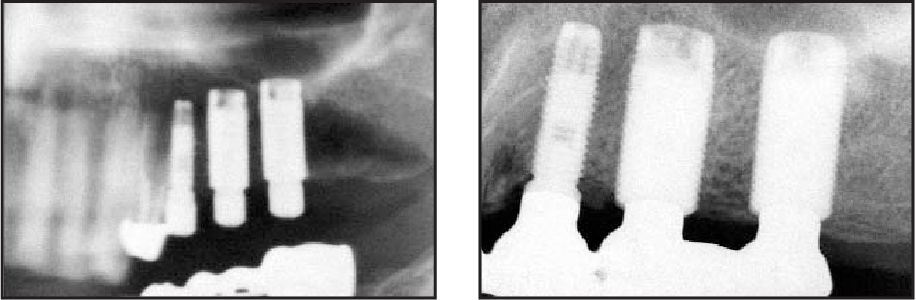
Why Is Platform Switching Important?
The concept of platform switching is aimed at minimizing vertical bone loss by providing different diameters of the platform and the abutment.
How Does It Work?
a. Inward positioning of the implant‑abutment interface allowed the biologic width to be established horizontally, as an additional horizontal surface area is created for soft tissue attachment.
b. The PS design increases the distance between the inflammatory cell infiltrate at the micro gap and the crestal bone, thereby minimizing the effect of inflammation on marginal bone remodeling.
c. Reduction in stresses, especially in the crestal region, by shifting the stresses away from the bone-implant interface.
The clinical advantages of this concept are as follows -
- Marginal Bone Preservation
- Increased implant longevity
- Reduced concentration of force on the crestal area.
- Improved esthetics
In the video below, you can see the reaction of two young periodontists watching, for the first time, a video showing early marginal bone loss around an implant without the Platform Switching concept.
Limitations Of Platform Switching
There exists a possibility of the deformation in the abutment/screw due to the concentrated stress on the junction of the abutment and platform. This calls for the need for stronger materials in the production of abutment and screws to prevent possible fracture during patient use.
If regular implants are to be used, smaller diameter abutments may compromise the emergence profile in aesthetic areas.
Around 3 mm of soft tissue should be present to place platform-switched implants or else bone resorption is likely to occur.
For platform switching to be effective, the under-sizing of the components must be carried out during all phases of the implant treatment.
How To Get Benefits Of Platform Switching
Gone are the days when clinicians had to choose components to platform switch the implant.
Most Implant companies today have PS integrated into the implant system itself.
Namely - Straumann, Nobel Biocare, Dentsply, Dentium, Osstem etc.
What Does Platform Switching Mean To Patients
A paradigm shift has occurred within health care to ‘patient‐centered’ care.
This has led to widespread agreement on the inclusion of patient‐reported assessments in dental research and practice.
Today are popularly known as patient‐reported outcome measures (PROMs).
In a recent PROM (Patient Related Outcome) study by Horwitz et al., patients experienced minimalistic pain and a high satisfaction with esthetics and function.
Indicative of overall patient benefit in implant therapy from platform switched implants.
Recent Scientific Standing
For a long time platform switching was considered to be the most effective way to achieve marginal bone preservation.
Riding the tide, almost all implant companies implemented platform switching as an essential feature of implant systems.
There are a plethora of studies showing the positive effects of platform switching.
However, recent clinical research conducted by Tomas Linkevicius group has shown that soft tissue thickness is a very critical factor in preserving crestal bone levels around implants.
They found that if vertical soft tissue thickness is 2mm or less, crestal bone resorption of 1.5mm occurs during the formation of a biological seal between soft tissues and implant-abutment/restorative surface.
Even implants with platform switched design could not maintain bone when vertical soft tissues were thin at the time of implant placement procedure.
This leads to the dilemma of what is more important:
Biology Or Implant Design?
With more such research in the future, there is hope for a better understanding of bone dynamics.
Conclusion
Marginal bone loss is a multifaceted problem, and thus, its solution cannot be attributed to any single factor.
Factors like depth of placement, vertical soft tissue height, presence of attached tissue, restorative material, abutment design, micro movement, emergence profile, etc., also need review.
Platform switching indeed has a biomechanical advantage, and its application in routine treatment aids in crestal bone preservation.
Though platform switching appears to be a promising tool, further research will justify its application in Implant Dentistry.
Questionnaire
Recommended Book: Contemporary Implant Dentistry
Comments
0 totalLoading comments...
Previous
Are all the implant surfaces the same? a review of the different surfaces.
Next
Tips and Tricks to Floss and Brush your Teeth Better
Related Articles

Dental KOL Marketing: How Implant and Periodontal Brands Build Their Key Opinion Leader Bench
11 min read
Dental Video Marketing: How Brands Use Clinical Video to Drive KOL Adoption
12 min read
